
MD, MPH, Executive Vice President, UNM Health Sciences, CEO, UNM Health
READ
MORE
MD, MPH, Executive Vice President, UNM Health Sciences, CEO, UNM Health
CLOSE
Nursing is a demanding profession in the best of times. The COVID-19 pandemic made it much, much harder. Here, nurses working at UNM Hospital and UNM Sandoval Regional Medical Center share their thoughts about their work, their motivation to serve and their dedication to achieving the best outcomes for their patients.
READ
MORE
CLOSE

Next door to The University of New Mexico Hospital, a 6.5-acre lot bustling with cranes and construction equipment will soon become the site of a new 96-bed adult critical care tower and 1,400-space parking structure.
The 570,000-square-foot New Hospital Tower, projected to open in Fall 2024, is needed to address longstanding overcrowding at UNMH by adding intensive care capacity, new operating rooms and a new emergency department.
The hospital is almost always on “Code Purple” status, meaning it is operating above capacity. Because available beds are already full, new patients can wait hours to be admitted.
Multiple factors contribute to the overcrowding.
UNMH is the only Level I trauma center in New Mexico, receiving patients from all over the state. As a tertiary care facility and teaching hospital it offers medical and surgical services that are unavailable elsewhere in the state, including the burn center, the UNM Children’s Hospital and the comprehensive stroke center.
The COVID-19 pandemic has exacerbated the problem, with a significant number of patients being transferred to UNMH for higher level care from elsewhere in New Mexico.
“I think the pandemic has highlighted that need for additional capacity, and it certainly would be helpful to have that capacity going forward,” says chief operating officer Michael Chicarelli, DNP.
At the pandemic’s peak, many patients had to defer surgical care until hospital capacity reached manageable levels. Additionally, many patients being admitted to the hospital now are sicker than expected, largely due to delayed primary and preventive care.
“We are in a crisis right now in New Mexico,” says Jennifer Vosburgh, DNP, RN, the hospital’s associate chief nursing officer. “The health care delivery system was not built for these current volumes. Patients are sicker, so they spend longer in the hospital and it takes longer for them to be discharged and free up a bed for another patient who is waiting to come in."
 Patient capacity is not the only challenge facing the hospital. Some parts of the facility are more than 60 years old, and an upgrade is long overdue.
Patient capacity is not the only challenge facing the hospital. Some parts of the facility are more than 60 years old, and an upgrade is long overdue.
“A hallway that was designed, say 50 years ago, is narrower and the floor to ceiling heights are shorter and the doorways are smaller,” says Michael E. Richards, MD, MPA, senior vice president for clinical affairs at UNM Health Sciences. “In some cases, we have difficulty moving equipment in and out of rooms.”
The New Hospital Tower, built to 21st Century standards, will provide long-needed enhancements.
Because the existing hospital was constructed in stages over decades, and many clinical services are located far apart, it can take as much as 20 minutes to walk from one service to another. When it comes to caring for someone with a life-threatening injury or disease, every second counts.
The New Hospital Tower has been designed to consolidate all adult critical care services under one roof. These services include 18 new operating rooms, 96 ICU beds and an emergency department with more than 40 exam rooms.
Additionally, the new parking structure – which will connect to the tower via a pedestrian bridge – will enable patients to reach medical services faster.
 The new facility includes amenities to enhance employee and patient well-being.
The new facility includes amenities to enhance employee and patient well-being.
One example is the addition of more natural light in the tower, which research has proven to immensely benefit patients and staff in health care settings.
The bottom line is the new tower – with its expanded emergency room and intensive care unit – will allow more New Mexicans to receive critical medical care in New Mexico.
“The planned hospital expansion is really important for us to continue providing the care that we have the honor of providing for the people of New Mexico, in New Mexico,” says Steve McLaughlin, MD, chair of the UNM Department of Emergency Medicine & Critical Care.
The completion of the New Hospital Tower is still a few years away, but in the meantime, for patients experiencing devastating injury or illness, UNMH will continue to deliver exceptional, quality health care to all New Mexicans.
To learn more, visit UNM Tower.
Dr. Cameron Crandall's legacy of working on behalf of the UNM Health Sciences LGBTQ community benefits providers -- and patients
READ
MORE
CLOSE

Cameron Crandall, MD, is dedicated to making institutional changes on behalf of the LGBTQ community because he wants to help others – starting in their doctor’s office.
“I don't really like to talk about myself,” he says. “I'd prefer to actually toil around the background and to make others successful. It's about serving our communities and giving everybody the opportunity to be successful.”
Crandall, who is gay, is the associate vice chancellor for LGBTQ Diversity, Equity & Inclusion in the UNM Health Sciences Office for Diversity, Equity & Inclusion, as well as vice chair for Research in the Department of Emergency Medicine. He also is a Regents' Professor in the Department of Emergency Medicine.
Crandall grew up in Seattle, attended the University of Washington and went on to study public health at Johns Hopkins University. He arrived in New Mexico in 1993 to train in emergency medicine, joined the faculty in 1996 and has been here ever since.
The role of associate vice chancellor for LGBTQ Diversity, Equity & Inclusion is unique not only in New Mexico but throughout the country, he says.
“There are . . . occasional physician champions or faculty champions in a number of different schools, but to have someone dedicated to addressing these issues I think is really unique, and I have to thank the leadership for having the foresight and the commitment to doing this,” Crandall says.
The administrator role allows Crandall to use his skills in public health research to examine health care disparities and LGBTQ health.
“A number of groups experience health care disparities and a large part of this work is to focus and work on addressing some of those issues from a systemic lens, rather than a one-on-one encounter,” he says. “It's important to do both, right? In the emergency department I provide direct care to patients, but it's also really important to recognize that you could also potentially do even greater good by making systemic changes by looking at our systemic patterns.”
Crandall also is faculty advisor and liaison for UNM LGBTQ Students and Allies in Healthcare (LSAH), a group dedicated to advancing the health of lesbian, gay, bisexual, transgender and queer people through community outreach, curriculum intervention, provider education and mentoring.
Under Crandall’s guidance, LSAH has worked to update the UNM School of Medicine curriculum so that future physicians and other providers are trained to ask more questions about a person when they come in for health care. LSAH is now working on bringing that throughout UNM Health Sciences to raise awareness and supply tools to address and recognize health care disparities among sexual and gender minorities.
LSAH created the curriculum using guidelines set by the Association of American Medical Colleges.
“After taking an inventory of the curriculum, we identified a number of different points of potential intervention and improvement in the curriculum,” Crandall says. The School of Medicine now has “a full curricular vision and map that identifies probably about 20 different points of intervention.”
Crandall says the group created the questions so that they don’t make assumptions about a person's sexual identity or sexual practices.
“If individuals are engaging in a particular form of sexual practice that might expose them to a risk, it's important to educate the patients on what those risks are and help them manage those risks,” he says.
“If you assume somebody is married, that it's a male and they're married to a woman, you shouldn't assume that the individual identifies as straight. They may actually have more than one partner. They may have sex with men or multiple partners. It's important to really delve beyond identity and really talk about sexual practices and behaviors.”
In addition to making impactful changes within education, Crandall also led the way in revamping the electronic health record within the UNM Health System.
“Early in my tenure of taking this position, there was an awareness about the substantial health care disparities that transgender and gender nonconforming or gender nonbinary individuals experience in . . . health systems,” he says.
That led to significant changes in rethinking and ultimately, revamping, the electronic health record to incorporate expanded notions of sexuality and gender, Crandall says. “We changed our basic core demographics, and we now allow individuals to tell us their sexual orientation, their gender identity.”
He’s also led efforts in developing and offering more classes for students and has found that teachers are learning along the way.
“And in some sense, I could even say it's a bit of a misguided effort in this way,” he says. “Our learners are more progressively minded and are much more aware of these issues than our teachers have been in many cases.
 “Sometimes what we really need to do is provide the tools to our teachers, because folks who are younger, in large, take variations in sexuality and gender for granted. And it's not as disconcerting or unusual for our learner age groups but when we have our teachers, oftentimes they struggle with the concepts. In that sense, it's not hard to teach the learners. They understand the material, they are hungry for more. They want more details, they want more specifics.”
“Sometimes what we really need to do is provide the tools to our teachers, because folks who are younger, in large, take variations in sexuality and gender for granted. And it's not as disconcerting or unusual for our learner age groups but when we have our teachers, oftentimes they struggle with the concepts. In that sense, it's not hard to teach the learners. They understand the material, they are hungry for more. They want more details, they want more specifics.”
In the not-too-distant future, Crandall would like to see UNM Health establish surgical services for transexual patients.
“We know New Mexico offers very few surgical services specific for trans patients,” he says. “I bring that forward, because in order to teach about those topics and people to learn about those topics you really need to be doing it. You can talk about neurosurgery, but if you don't have a neurosurgeon, you're not going to learn much about surgery. So, if you're not doing some of these procedures and have the patients and the skill set to work around these patients, from a multidisciplinary model, it really falls flat.”
He also envisions UNM changing how it collects personal information, so that identifying sexuality and gender minority status is part of the process for applicants, whether it’s for students, staff or faculty.
“We need to do it because we'll use that information to ensure that we're doing the best we can for all of our groups of students and communities,” he says.

Jan Martin leads a new UNM College of Nursing partnership with Bernalillo County to help train family caregivers
READ
MORE
CLOSE
 Your new job started yesterday, when your grandmother was discharged from the hospital after a life-altering stroke.
Your new job started yesterday, when your grandmother was discharged from the hospital after a life-altering stroke.
You’ll be helping her around the house, ensuring she gets the right medicine at the right time and helping her get to a plethora of doctor’s appointments. You have no experience in health care – besides those few times you nursed fevers or dutifully picked up your still groggy loved one from surgery, but you will work an average of 18 hours a week caring for her, and you will receive no training and no compensation. On top of that, you still need to keep all the other aspects of your daily life afloat.
Each year, one in five New Mexicans serves as a family caregiver, providing this type of long-term, in-home care, according to the to the New Mexico Aging & Long-Term Services Department.
Starting in February 2022 The University of New Mexico College of Nursing and the Bernalillo County Office of Senior and Social Services partnered to launch the Caregiver Training Program, which works to support older caregivers and caregivers of older adults, providing them with an individualized program to empower them to best care for their loved one and for themselves.
Until now, there have been no training programs in New Mexico for people with little experience providing health care who must suddenly transition into a primary caregiver for someone with unique medical needs.
“There is a huge percentage of New Mexicans that dedicate a huge chunk of their lives in unreimbursed, unsupported family caregiving, and we need to take care of them as well,” said Jan Martin, DNP, an associate professor and interim assistant dean for clinical affairs in the College of Nursing.
The program provides individualized assistance and training to address each caregiver’s unique situation. A registered nurse with experience in providing in-home geriatric care completes an initial assessment and meets with a caregiver to understand what their day is like, how they assist the person they are caring for and any difficulties they experience in providing that care.
After the assessment, the nurse works with the caregiver to develop a plan to help strengthen skills and provide support. That can include education about medications or learning movements to bathe or move a person to ensure neither the caregiver nor the person they are caring for is injured. It can also include support in finding community resources to assist with food, housing or transportation, or helping a caregiver find respite to get a break and time to recharge.
The referral-based program is expected to train 50 caregivers in its first year.
The program grew out of Albuquerque’s Geriatric Education and Health Maintenance Clinic, which provides education, resources and basic preventive health care to seniors in pop-up clinics in senior centers around the city.
Nursing students will also participate in the program as part of their clinical rotations. Under supervision of a registered nurse, students will be paired with a client for seven to 16 weeks.
This program provides students an opportunity to learn about home health care and working with older adults outside of a hospital or assisted living setting. It is expected to build student nurses’ skills in conducting assessments, creating and maintain safe home environments for clients and talking to people about medications and maintaining good health.
Martin hopes that this program allows students to see the outcomes of the care they provide and develop a stronger connection with caregivers and clients.
“It's really important for our students to see that continuity and develop that relationship with a client, because then they can also see, ‘Oh, wow, I did this,’” she said. “It's important for them to see the value of what they do. They're not just out there learning, they’re actually assisting someone else and are can see the difference they make.”
The program hopes to address an unmet need in the community.
Family caregivers provide 80% of all long-term care in the United States, according to the Aging & Long-Term Services Department. Each year, 419,000 New Mexicans provide more than 274 million hours of unpaid family care, often with little to no training in how to provide that care, while still taking care of themselves. On average, these family caregivers dedicate an average of 18 hours a week to care tasks.
Demand for family caregivers is also expected to rise as the state’s population ages. New Mexico’s 80 and older population is projected to grow by 81% by 2030.
READ
MORE
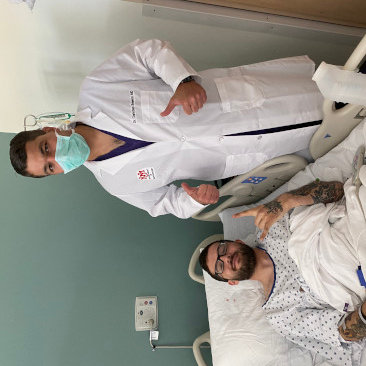
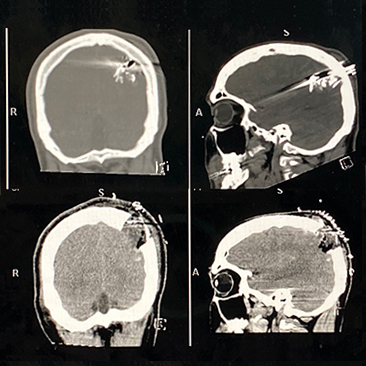
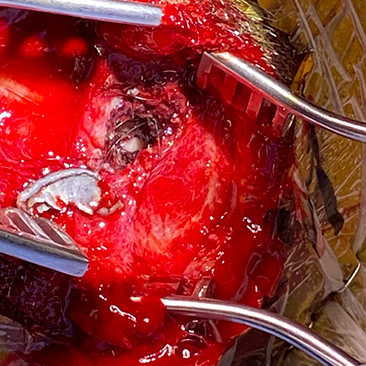
A neurosurgeon reflects on a patient's close call with disaster [Warning: graphic image]

I grew up obsessed with sports.
One of my favorite things about sports is that contests are won or lost on the thinnest of margins. A single millimeter can be the margin of victory or defeat, and that same margin is just as true in the "real" world.
In medicine – and especially in trauma and neurosurgery – survival, life and death, or the difference between permanent impairment or normal full recovery, is also a matter of millimeters.
Last spring, my patient was struck in the back of his head with a bullet while driving. Miraculously, the bullet traveled one of the only narrow paths in the back of the brain that is somewhat safe.
Had the bullet penetrated a few millimeters deeper, he would have died. If the bullet had traveled a few millimeters higher and more to the front, he would have been left permanently paralyzed. A little more toward the middle of the brain and he would have lost half his vision.
The path the bullet took was truly miraculous! This amazing young man had the best outcome possible.
I'm grateful for our amazing trauma team at UNM Hospital – so many lives saved by the state's only Level I trauma center! I am grateful for small part we are able to play in saving our patients.
Life, like sports, is a game of millimeters. We must always give our best, because the margins between success and failure, life and death, normal full recovery or permanent impairment, are razor thin and often composed of a few millimeters.
So our best effort allows us to focus on what we can control, and pray to God and hope for the best with all the things out of our control.
READ
MORE
CLOSE
 On a steep slope just below Sandia Crest a group of physicians, nurses, paramedics and physician assistants have gathered beneath a canopy of aspens and spruce to learn about high-angle wilderness rescue.
On a steep slope just below Sandia Crest a group of physicians, nurses, paramedics and physician assistants have gathered beneath a canopy of aspens and spruce to learn about high-angle wilderness rescue.
It’s an exercise in ropes and trust.
Trevor Mayschak, a paramedic and senior lecturer in The University of New Mexico’s International Mountain Medicine Center, and his colleague Angela Martz, a physician’s assistant, are demonstrating how to anchor and rig climbing ropes for hauling injured people to safety.
Martz demonstrates how, with the use of an intricate series of pulleys and knots, she can move Mayschak up the slope with minimal effort.
A few feet farther down, the ground abruptly drops away – a 30- or 40-foot drop. “People do occasionally fall over this cliff band and need rescue,” Mayschak says matter-of-factly.
He quizzes the group, shivering in the morning air at an elevation of nearly 10,600 feet, about the best trees to use as rope anchors (he advises against aspens, which have shallow root systems). “As far as anchors go, not great,” he says. “Don’t just settle for something that’s large and is convenient."
The group of 18 medical providers – most from out of state – are midway through a nine-day summer course on their way to earning a diploma in Mountain Medicine. During their visit, they will practice procedures for treating and transporting injured patients in remote settings, along with assorted alpine skills and helicopter rescue techniques.
Most of the participants already have some experience in wilderness rescue, Mayschak says later.
“We require a real base level of expertise, so when we put them in the terrain they’re not overwhelmed,” he says, noting that the course intermixes technical mountaineering skills with a focus on providing care in austere environments. “The end goal is for them to integrate both aspects into a rescue operation.”
UNM first received international accreditation for its austere and mountain medicine program in 2011, and the International Mountain Medicine Center was established in 2016 within the UNM Department of Emergency Medicine, says Jason Williams, the center’s director.
The Mountain Medicine diploma is one of only a few offered in the U.S., Williams says, and in 2017 the program began collaborating with the Bernalillo County Sheriff’s Office helicopter rescue team – which sets it apart, enabling rescuers to reach and retrieve people from inaccessible locations. “We’re the only program in the U.S. that has that robust a helicopter component,” he says.
Today, the center has a full-time staff, along with eight affiliated physicians and physician assistants. The diploma program has summer and winter components, along with a robust online learning component, he says.
Aaron Reilly, DO, an emergency physician at UNM Sandoval Regional Medical Center, also serves as medical director of UNM’s Reach and Treat team, which assists in wilderness rescues throughout New Mexico. Typical back country emergencies include musculoskeletal injuries from climbing accidents and falls, fatigue, dehydration and hypothermia, he says.
The priority in treating injuries in the wild is to safely and rapidly evacuate a patient so they can receive proper treatment. “Medicine is the same regardless of where you are,” he says. “You’re going to do things a little bit differently than when someone comes into the emergency department.”
Blair Anderson, a flight nurse from Morganton, N.C., started out volunteering with a local fire department and fell in love with wilderness rescue. She learned about the UNM course from a friend who went through it two years ago.
“I’ve enjoyed the hands-on part,” she says. “This is the highest altitude I’ve ever been at.”
Jason Williams says he and his colleagues look forward to getting into the mountains whenever they can. “They share a love of the outdoors and medicine and we mix it together – and they’re really happy,” he says.


Christian Bowers, MD, associate professor, UNM Department of Neurosurgery
“I have three main purposes for my account. I want to show people the high-quality neuro-oncology/ brain tumor work that we do here at UNM. I want to teach patients before surgery. I show them videos of previous cases, etc., and then they use it as a resource and learn about the surgeries that I do. I’m also trying to highlight our research and build a following with medical students, since that is a big area and focus for me.”
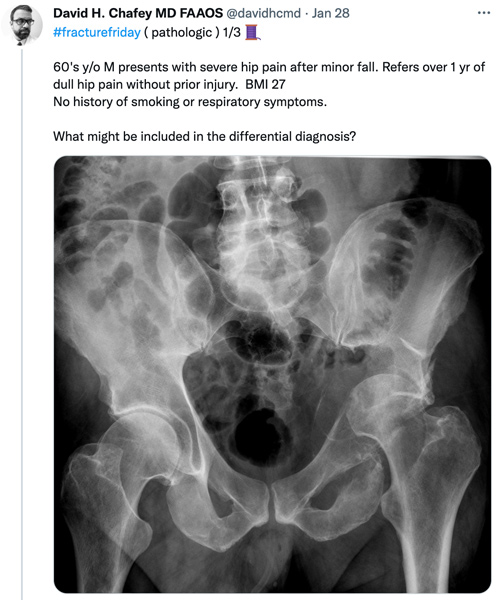

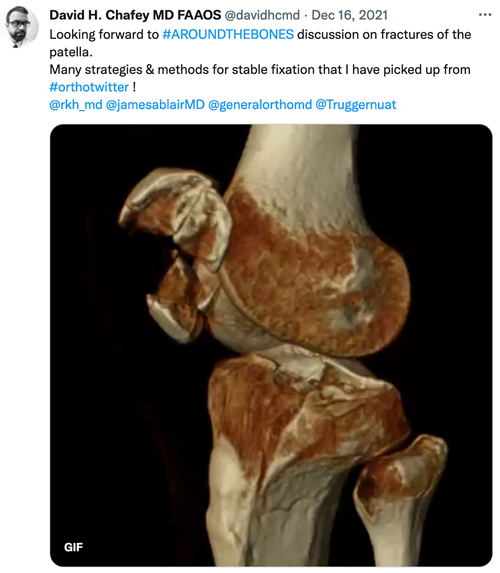

David Chafey, MD, associate professor, UNM Department of Orthopaedics & Rehabilitation
“I joined Twitter because I was in one of our professional associations and I became the program director for an event. It opened up a lot of networking connections that became even more valuable during the pandemic and we weren’t able to travel. The old ways of staying connected and meeting people at a conference and networking were just not as available. I use Twitter for education, advocacy and mentoring. It’s opened real-world opportunities for me. I’ve given virtual lectures in three countries. I have pending invitations to travel, thanks to those opportunities. I’ve had students connected with other students.”
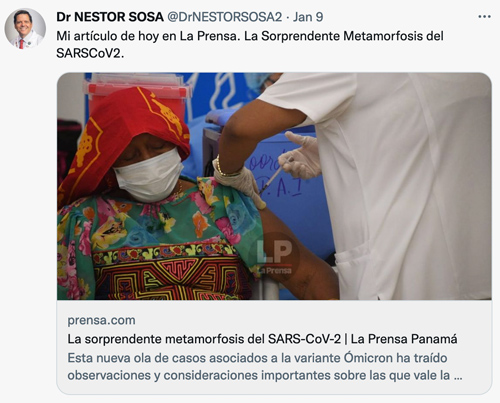
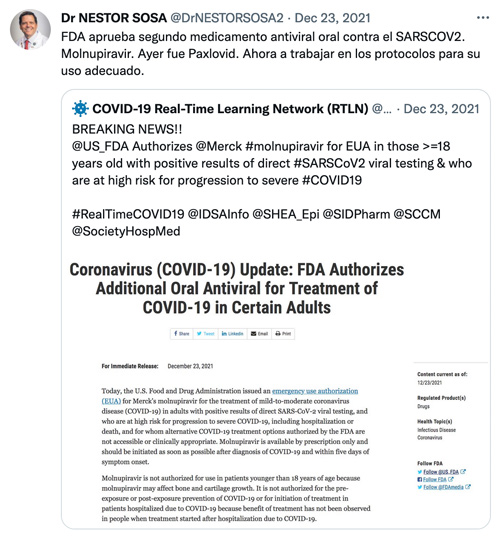



Nestor Sosa, MD, Chief, UNM Division of Infectious Diseases
“My main audience is from my country Panama, so the great majority of my posts are in Spanish. Most of what I post is related to education, centered on the pandemic, to combat misinformation and to clarify important scientific or public health messages. I participate regularly in TV interviews for Panama and I write a monthly op-ed on medical and scientific topics in Spanish for the most important paper in Panama, so I usually retweet clips from these interviews and publications to enhance the educational effect.”
For one student, a degree in Population Health affords an opportunity to serve the health needs of her fellow New Mexicans
READ
MORE

CLOSE
The uncertainty of the pandemic may have changed various things about my life, but I’ve known I always wanted to go into health care. I was able to finish high school a year early, and also received my associate of arts in liberal arts from San Juan College in Farmington, N.M., in May 2020.
I started the process of applying to colleges in October 2019, but I was certain that I wanted to attend UNM. My mom is a UNM graduate, and watching her receive her master’s degree has been my inspiration to further my education. When I wanted to decide on a major, I began researching on the UNM webpage. I saw “Population Health,” and was curious about it.
When I attended my tour at UNM, I spoke to my current academic advisor, Danny Noreiga-Lucero. He shared more information about the degree program, and I knew it would be the perfect degree for me.
My favorite thing about being in the College of Population Health is working with instructors who are truly experts in their field. I appreciate that the courses are very diverse and truly represent the field of population health. I’ve been able to learn epidemiology, public policy, population health biology, health care finance, and so much more. The class sizes are small, and you are able to move through the program with your classmates. I have built strong connections that I will take into my future career.
After I receive my bachelor of science in Population Health in December, I plan on applying to the UNM Physician Assistant program. I would like to work as a psychiatry provider in the underserved areas in the state, to address opioid and alcohol-use disorders. The College of Population Health has provided me with skills to address the various areas of health, and the passion to serve in New Mexico.
READ
MORE
Dr. Rita Serda is on a quest to activate the immune system to seek out and destroy cancer cells -- and it could be a game-changer
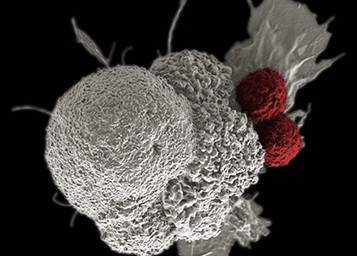
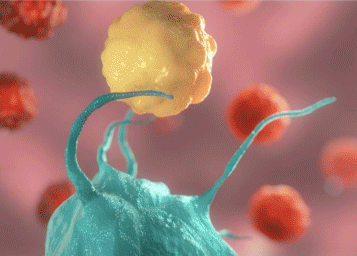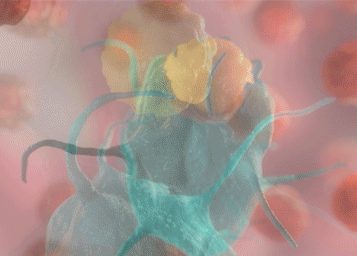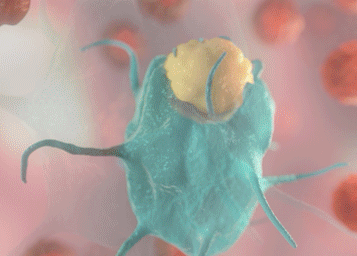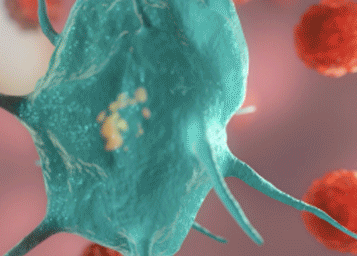
During her graduate studies at The University of New Mexico, Rita Elena Serda, PhD, worked with a professor who died of cancer. That experience made her think about how she would want her loved ones to be treated if they were ever diagnosed with cancer.
“I would want something that would get rid of all the cancer,” she says. And so she focused her research on immunotherapy.
“If you’re able to get the body to make an immune response to kill cancer,” she says, “that’s your chance to get rid of all those metastatic cancer cells, the ones that we can’t control right now.”
After earning her doctorate from UNM, Serda worked at Houston Methodist and Baylor College of Medicine in Texas. There, she developed porous nanoparticles that activated the immune system using photolithography techniques on silicon wafers.
Serda returned to New Mexico 10 years later and worked with Jeffrey Brinker, PhD, and Sarah Adams, MD, at the UNM Comprehensive Cancer Center. Using Brinker’s nanoparticle fabrication process and ovarian cancer cells that Adams obtained, Serda developed new methods to make immunotherapy silica nanoparticles and to preserve cancer cells using the mineral silica.
Cancer cells notoriously evade the immune system by disguising themselves as benign objects. Weakened immune systems allow disguised cancer cells to grow and multiply, and they also struggle to rid the body of cancer because – even within the same person – a single tumor can have cancer cells that differ in their mutations.
“Cancer is different from person to person and even within the same person,” Serda says. “We can’t target just one protein because there are different mutations in different cancer cells.”
Serda’s personalized immunotherapies simultaneously reveal cancer cells to the immune system and embrace their heterogeneity.
To make her cell-based immunotherapy, Serda coats a patient’s cancer cells with silica, then alters the particles’ surfaces to make the immune system take notice. Her process preserves the cancer cells’ proteins and activates the body’s immune cells, which is the key to their effectiveness.
Normally, dendritic cells in the immune system act as scavengers, Serda says. They find and internalize foreign cells, break them down, and then show the pieces – called antigens – to immune system T-cells, thus activating them.
The T-cells then multiply and roam through the body. When they recognize a foreign cell, they eliminate it by killing it directly or by inducing it into a controlled self-destruct process called apoptosis.
In her most recent study published in Nature Biomedical Engineering, Serda and her team showed that dendritic cells engulf the silicified cancer cells whole. Their images also showed that the cancer cell within each silica particle remains intact until the dendritic cell breaks it down.
“Imaging is super-important to me,” Serda says. “It gives me a lot of motivation in my research.”
Using histology, fluorescence microscopy and flow cytometry shared resources through the UNM Cancer Center, Serda’s team was able to isolate dendritic cells and take scans of them. Using the scans, they created three-dimensional representations that allowed them to take cut-away images that show the intact silicified cells within a dendritic cell before the dendritic cell dismantles it.
The unique cancer antigens that dendritic cells present to T-cells enable the T-cells to recognize that type of cancer cell. And because each silicified cell has different cancer antigens, the immune system can be trained to recognize the vast array of cancer cells in that person.
But Serda found simply coating cancer cells with silica wasn’t always enough to spur a cancer-tolerating immune system to action. She needed a way to ensure that the silicified cells would produce a strong response, so she turned to microbial molecules.
Serda attached bacterial molecules to the silicified cell surfaces, making them look like bacterial cells. In the article, her team showed that this addition induced a much stronger response from the immune system.
Serda’s preclinical studies show that once a strong immune response is induced, the immunity lasts a long time. These studies were conducted in mice using mouse cancer cells.
The next step, Serda says, is to demonstrate that the silicified cells are safe for people. Although she is working with her company, Enchantment Pharmaceuticals, and the U.S. Food and Drug Administration to develop the testing plan, the first clinical trials are still some time away.
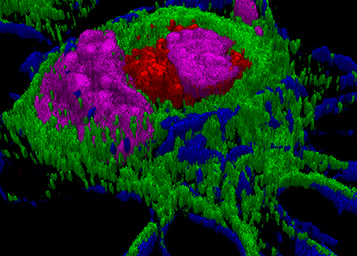
Many of Serda’s scientific images are publicly available through the National Cancer Institute (NCI). One image won the NCI Cancer Close Up competition and was published in the The Washington Post. Another adorns a postage stamp. The striking images show immune cells attacking cancer cells and either gobbling them, killing them, or inducing apoptosis in them.
“I love photography and imaging,” Serda says. Capturing images as she’s conducting research motivates her. “It’s my way to be artistic in the lab.”
“Cancer vaccines from cryogenically silicified tumor cells functionalized with pathogen-associated molecular patterns” was published in the November 1, 2021, online edition of Nature Biomedical Engineering. Authors are: Jimin Guo, Henning de May, Stefan Franco, Achraf Noureddine, Lien Tang, C. J. Brinker, Donna F. Kusewitt, Sarah F. Adams, and Rita E. Serda. The work was supported by UNM Comprehensive Cancer Center, NIH grant NCI P30118100 (PI Willman, C.), and also by AIM center, NIH grant P20GM121176.

UNM College of Pharmacy students team up to educate the public about the dangers of addiction with Operation Substance Abuse
READ
MORE

CLOSE
 Operation Substance Use Disorder is an initiative led by students in The University of New Mexico College of Pharmacy that aims to educate the public about any substance that may be abused or misused. This includes physical dependence, mental dependence, alcohol misuse, opioid misuse and tobacco misuse, as well as illegal substance misuse.
Operation Substance Use Disorder is an initiative led by students in The University of New Mexico College of Pharmacy that aims to educate the public about any substance that may be abused or misused. This includes physical dependence, mental dependence, alcohol misuse, opioid misuse and tobacco misuse, as well as illegal substance misuse.
Our team consists of three third-year Pharmacy students: Devin Signs, Jovena Cleary and myself. I joined the project because of the prominent impact that it has on the community.
We have had events at Walmart, where we discussed with members of the public the reason why medications need to be discarded safely. We have also reached out to numerous patients and have seen their enjoyment from the knowledge that they gained.
My first-hand experience with the substance use disorder initiative has been wonderful. I have seen the thrill in students when we discuss the opportunity of getting them trained in naloxone administration, for example.
 Substance use disorder in New Mexico is at epidemic levels. We have an overuse of alcohol, opioids, cannabis and virtually all other substances. With the knowledge that I have gained in my education, as well as through this initiative, I have been able to talk with family members, colleagues and students about the importance of this problem.
Substance use disorder in New Mexico is at epidemic levels. We have an overuse of alcohol, opioids, cannabis and virtually all other substances. With the knowledge that I have gained in my education, as well as through this initiative, I have been able to talk with family members, colleagues and students about the importance of this problem.
We need to continue to work at educating the public on the prevalence of these different substances being abused. High school and college students abuse alcohol to address their stress.
In our outreach, we have also been addressing stress management. We are working to educate the public on utilizing different techniques to cope with stress. Instead of turning to alcohol, they might try exercise, meditation or communicating with friends.
With education comes knowledge. Instead of trying to educate the public with scare tactics, we can express our concern through education and helping the public understand why we care about their well-being. The public will grow in knowledge, which will enable them to educate their family members and friends.
 From first-hand experience I have come to see the importance of educating the public on substance use disorder.
From first-hand experience I have come to see the importance of educating the public on substance use disorder.
There is too little awareness about what it means to have a substance use disorder, and there is little knowledge of how a substance forces the body to become physically dependent upon it.
We will continue to work towards fulfilling our state’s needs when it comes to the abuse of substances.
READ
MORE
The University of New Mexico Center for Adult Critical Care uses an innovative model to bring together specialists from across disciplines to save lives



CLOSE
The University of New Mexico Center for Adult Critical Care uses an innovative model to bring together specialists from across disciplines to save lives
Physicians often speak of the “golden hour” as a window to provide lifesaving care for patients brought an emergency department. At UNM Hospital’s busy Level I trauma center, that care is provided by a highly experienced team of doctors, nurses and techs.
What comes next – a period sometimes described as the “silver day” – is equally important, as very sick patients are transferred to intensive care to be treated by physicians from the UNM Center for Adult Critical Care.
“If, in that first 24 hours, you don’t get resuscitated, your 30-day mortality is massively higher,” says Jon Marinaro, MD, professor and co-chief, along with Michelle Harkins, MD, professor in the Department of Internal Medicine, of the Center for Adult Critical Care.
Resuscitation, in this case, means managing multiple conditions and restoring full function to the patient’s organs while staving off renal, brain and lung failure, Marinaro says.
The Center for Adult Critical Care is a unique interdisciplinary resource, bringing together 55 critical care doctors from six departments in the UNM School of Medicine: Anesthesia & Critical Care Medicine; Surgery; Internal Medicine; Emergency Medicine; Neurosurgery and Neurology.
First established in 2015, the center’s organizational model enables physicians from different specialties who train and work together to address patients’ acute medical needs – and that translates into better outcomes, Marinaro says.
Harkins agrees. "With the diversity in our training, we can learn from each other and provide excellent critical care," she says. "We're a much more collaborative group than we've ever been before."
Team members meet periodically to review statistics and metrics and build interdisciplinary bridges. "Working together as a team we can meet the needs of the patients," she says. "At other institutions it’s much more territorial. We’re in it together to take care of the patients.”
Steve McLaughlin, MD, chair of the Department of Emergency Medicine, says UNM Hospital, with the only Level I trauma center in the state, has several unique features that contribute to a deep talent pool in critical care.
“The fact that we’re a trauma center, and the fact that we’re the referral center for all of the really complicated and sick patients in the state of New Mexico, creates a concentration here of both patients in our care, but also providers who are really committed to providing that high level of trauma care and high levels of other types of critical care,” he says.
“That’s really allowed us to focus on it at the institution, and I think the mission of the institution is one of the things that has attracted so many talented people. Our intensive care group here is really phenomenal. We’re recruiting people from some of the best programs in the country to come here to New Mexico to be part of this group.”
Adds Marinaro, “Critical care at The University of New Mexico has really come into its own.”

Researchers at New Mexico's only academic health center have launched more than 137 studies – including 24 clinical trials – related to the COVID-19 pandemic
READ
MORE

CLOSE
Two years into the COVID-19 pandemic, The University of New Mexico Health Sciences Center has drawn on its strengths as an academic health center to launch more than 137 studies – including 24 clinical trials – related to the SARS-CoV-2 coronavirus.
The work spanned the spectrum, from characterizing emerging genomic variations in the virus and evaluating COVID safety protocols in clinical settings to computational analyses of existing drugs for potential antiviral therapeutics.
Two studies in particular stood out for their impact on the wider community: a national trial of the Moderna vaccine in children 12 and under and a National Institutes of Health-funded study of patients with lingering “Long COVID” symptoms the Researching COVID to Enhance Recovery (RECOVER) Initiative.
 The projects, coordinated through the UNM Clinical & Translational Science Center (CTSC), drew on the HSC’s demonstrated ability to enroll a diverse patient cohort, including Hispanic and American Indian participants, said Hengameh Raissy, PharmD, the vice chair for research in the Department of Pediatrics, who serves a co-principal investigator for RECOVER and leads the CTSC’s Network Capacity.
The projects, coordinated through the UNM Clinical & Translational Science Center (CTSC), drew on the HSC’s demonstrated ability to enroll a diverse patient cohort, including Hispanic and American Indian participants, said Hengameh Raissy, PharmD, the vice chair for research in the Department of Pediatrics, who serves a co-principal investigator for RECOVER and leads the CTSC’s Network Capacity.
“Minorities have historically been underrepresented in clinical research trials,” Raissy said. “Our goal is to enroll to include diversity in the study populations in order to have generalizability of research to the population.”
The Moderna vaccine KidCOVE trial started by enrolling 65 New Mexico children ages 6 through 12, said Walter Dehority, MD, MSc, an infectious disease specialist and associate professor in the UNM Department of Pediatrics who serves as principal investigator for the study.
Vaccinating children “has huge implications for the opening of schools,” he says. “A lot of teachers might not feel comfortable going back to in-person learning, but they might if they knew the children they were teaching were immunized. The same would apply to other youth activities, such as sports."
Dehority points out that even if the most severe impact of the disease is seen in adults, some children do become seriously ill.
“During the COVID epidemic we’ve had four or five kids in the hospital at a given time, and they’re often in the intensive care unit,” he says. “Why have New Mexican kids in the ICU with COVID-related disease every day if we could prevent that?”
Additionally, having children vaccinated will also make adult family members who might be at risk for COVID (such as grandparents) more comfortable and safer when they are around the youngsters.
UNM is one of dozens of sites around the country participating in the KidCOVE study, which aims to enroll close to 7,000 children and follow them for about 14 months, Dehority said.
In the randomized, double blind controlled study children receive either a placebo or the first dose of the Moderna mRNA-1273 vaccine when they enroll, then return about a month later for the second shot, he said.
Parents and children are asked to return to the UNM CTSC clinic for follow-up testing in subsequent months, and there will be at least two visits with the research team after each injection.
The next two phases of the trial, which are expected to start later in the fall, include children ages 6 months to 5 years old.
Additional co-investigators on the study include Raissy and fellow Pediatrics faculty members Chandler Todd, MD, and Matthew Kadish, MD.
Starting last spring, NIH invited academic health centers to develop protocols for the RECOVER study, which hopes to enroll more than 17,000 patients at institutions around the country to study Long COVID -- also referred to as Post-Acute Sequelae of SARS-CoV2 (PASC).
The UNM Health Sciences Center expects to enroll 200 adults and 200 children, including people already experiencing symptoms and those newly diagnosed with COVID-19, Raissy said.
According to NIH, Long COVID symptoms may include ongoing fatigue, shortness of breath, “brain fog,” sleep disorders, fevers, gastrointestinal symptoms, anxiety and depression. Symptoms can persist for months, ranging from mild to incapacitating. In some cases, new symptoms arise well after the time of infection or evolve over time.
The studies seek better understanding of how many people continue to have COVID-19 symptoms (or develop new symptoms) and what the underlying biological causes might be. This could provide insight into what makes some people vulnerable to these symptoms – and whether they increase the risk for other conditions, such as chronic heart or brain disorders.
“It’s trying to ascertain who develops PASC,” said Michelle Harkins, MD, professor of Internal Medicine and co-principal investigator on the adult study. "Are there treatments that actually mitigate it at the beginning or help with their symptoms later?"
The studies will include a close review of medical records, as well as extensive diagnostic screening, such as blood tests and CT and MRI scans, to gather as much information as possible about each patient and their symptoms, Raissy said.
“This is a huge collaboration between the Clinical & Translational Science Center, which applied for the study, UNM Hospital and the Departments of Pediatrics, Internal Medicine, Neurology, Emergency Medicine and Psychiatry & Behavioral Sciences,” she said.
Other investigators for the adult study include Alisha Parada, MD, associate professor in Internal Medicine, Davin Quinn, MD, professor in Psychiatry & Behavioral Sciences, and Elyce Sheehan, MD, assistant professor in Internal Medicine.
Walter Dehority is co-principal investigator on the pediatric arm, with additional investigators Matthew Kadish and Jerry Larrabee, MD, MEd, professor of Pediatrics.

Project ECHO has a unique vision for improving health outcomes in communities all over the world
READ
MORE
CLOSE
Project ECHO, The University of New Mexico’s signature tele-mentoring initiative, has an impressive track record of delivering effective interventions that have improved health outcomes in communities all over the world.
Starting in September 2020 – at the height of the COVID-19 pandemic – ECHO executed a 12-month program on behalf of the Agency for Healthcare Research and Quality (AHRQ) to work with U.S. nursing homes to reduce the spread of the coronavirus in their facilities.
“This is an amazing project,” said Nancy Hood, ECHO’s director of research and evaluation. According AHRQ data, ECHO’s 99 partner hubs offered training to 9,058 nursing homes – 59% of 15,400 facilities that were eligible.
The aim was to provide a curriculum designed by the Institute for Healthcare Improvement to reduce the risks to some of the most vulnerable people. Nearly 32,000 nursing home staff participated, and the facilities participating were home to about 1.7 million residents.
“The most exciting thing about the nursing home project was it retained the small, two-way interaction, providing peer-to-peer learning in a safe, trusting environment,” Hood said. “This was an environment where they could learn from each other and talk about their challenges and get the most up-to-date information.”
Joanna Katzman, MD, medical director of Project ECHO’s Pain, Substance Use and Public Health Program, is an expert in reducing reliance on medications to treat chronic pain. She partnered with the Defense Health Agency in a four-year project to train Army and Navy medical providers in pain management and opioid prescribing.
Patients where clinicians received the training saw a marked drop in the number of new opioid prescriptions being written for their patients, compared to patients whose providers had not received the training. “The doctors who were being trained via ECHO were not writing new opioid prescriptions and not getting them started on this whole course of treatment,” Katzman said.
The patient pool ranged from age 18 to 64, females and males, seen at military health care clinics around the globe. “We studied not only active military, but beneficiaries, dependents and retirees,” Katzman said. “We tried to present an integrative approach. The goal is not to just teach why opiates are bad to give doctors alternatives about how to handle these patients.”
She adds, “By training clinicians you can change provider behavior, which then can affect patient care. That’s really what we are showing.”
UNM pulmonologist Akshay Sood, MBBS, MPH, who specializes in treating miners for black lung disease and pneumoconiosis, worked with Miners’ Colfax Medical Center in Raton, N.M., to create a tele-ECHO to train rural clinicians to care for a surge of new patients.
“The program provides longitudinal tele-mentoring to professionals taking care of miners,” Sood said. “It focuses on underserved populations and it serves a rural need that’s emerging. To the best of our knowledge, it’s one of the few programs that focuses on occupational diseases.”
Following sessions that unfolded over a 12-month period in 2018 and 2019 participating clinicians, care providers and others reported significantly greater self-efficacy in treating miners’ lung disease.
The program was “a genuine partnership between a university and rural community health institution,” Sood says. “There’s no one institute that has all the skillsets required to take care of miners.”
It also helped that the presentations were provided by experts in New Mexico.
“Knowledge transfer coming from rural areas is more effective than knowledge transfer coming from urban areas,” he said. “ECHO is a very powerful tool for people in rural areas.”
Amid widespread skepticism and uncertainty, a mother weighs whether to enroll her toddler in a COVID vaccine trial
READ
MORE

CLOSE
The clock says 11:30 p.m.
I have only been asleep two hours, but I am suddenly wide awake – and it’s more than the snoring of my child coming through the baby monitor that has my brain energized. It’s the thought that in a few hours I will take my 2-year-old, the most precious thing I have in the world, to a research facility to be part of the Moderna COVID vaccine trial.
I open my emails and scan to find the electronic consent form sent to me days earlier. I know what’s in the 32 pages already – child will receive a quarter of an adult dose, common reactions include rash, soreness and fever, etc. Then there is the section on rare reactions. Myocarditis and pericarditis – heart inflammation – is mostly seen in preteen and teenage boys. I know that it’s very rare and that every case seen so far has resolved itself naturally, but all that goes out the window when I think of my child and his safety.
Right about the time my breathing is picking up, I stop and close my eyes. I believe in science, I have been vaccinated – eight months pregnant, no less, with our infant – my husband is vaccinated, and the risks of COVID are greater than the vaccine. It’s funny to say, but repeating the facts I know about the vaccine in my head comforts me.
It feels like the blink of an eye between lying in bed repeating those facts to myself and opening the clinic doors and signing in. “We are here for the Moderna trial,” I say, trying to balance my purse, diaper bag and a 2-year-old who insisted on being carried.
Back in the room, a research coordinator comes in and introduces herself. She will be my partner in this and oversee my son’s participation the trial. She’s patient with me and I am grateful. I ask a few questions and confirm I have read the consent form. I leave out that I have read it about a hundred times.
Physical exam, nasal swab, blood draw – and then the big moment. She goes over the order and what to expect. Her delivery is comforting, and even though she tells me she doesn’t have kids, it’s clear she cares deeply about children and the children in this trial.
“One hundred and fourteen,” she tells me. That’s his number – my sweet, Paw Patrol-loving little boy will be identified as this number for the next 394 days, the length of the trial.
UNM Health Sciences is only one of 88 sites selected to conduct these trials in children. They have already had a successful cohort in kids 5-11 before the Food and Drug Administration (FDA) approved the Pfizer vaccine for emergency use a few weeks ago. Children 6 months to 5 years are next – and that’s how we ended up here today. As an employee of UNM I have been excited for this trial, but as a mother it’s scary.
The shot is quick: a few tears and then he is fine, going right back to watching his tablet and playing. There is a 3-out-of-4 chance the syringe contained the Moderna vaccine, with the placebo being just saline solution. We won’t know for more than a year, but I will be on the lookout over the next few days for the telltale signs he got the real deal.
This overwhelming sense of relief comes over me. I know I did the right thing for my child. I consulted his pediatrician and trusted her advice. I also know that our hospitals are full and everyone doing their part to get vaccinated and reduce the spread and mutation of COVID is critical.
As I tuck him into bed, I tell him the same thing he hears every night: “Mommy and Daddy love you so much.” For some reason tonight it sounds deeper. I want him to know that we took every step possible to protect him during this global pandemic – even when it was scary and controversial to do so.
So, from one mother to any parent out there, talk to a doctor you trust, try to avoid misinformation on social media or the internet, and make the decision that’s best for your child.
Remember, your parents didn’t have to raise kids in a global pandemic. You are doing a great job, so be kind to yourself. We all love our kids and want the best for them. For me, the best is the COVID-19 vaccine.
The author is not revealing her name to protect the identity of her child. She is an employee of The University of New Mexico. All opinions in this piece are those of the author and do not necessarily represent UNM.
How UNM’s International Mountain Medicine Team Helped Stranded Sandia Tram Passengers Reach Safety
READ
MORE
How UNM’s International Mountain Medicine Team Helped Stranded Sandia Tram Passengers Reach Safety
CLOSE
 Workers who had just ended their shift at the Ten 3 restaurant late on New Year’s Eve 2021 were bundled up against howling wind and snow as they stepped aboard a tram car atop Sandia Peak for the 15-minute trip down the mountain.
Workers who had just ended their shift at the Ten 3 restaurant late on New Year’s Eve 2021 were bundled up against howling wind and snow as they stepped aboard a tram car atop Sandia Peak for the 15-minute trip down the mountain.
Minutes later, the car ground to a halt, suspended a thousand feet above a rocky canyon as a thick coating of ice on the steel tram cables prevented it from moving any farther. Twenty people were huddled in one car, and a lone employee was in the other.
It was still dark when Trevor Mayschak, a paramedic and senior lecturer at The University of New Mexico International Mountain Medicine Center, got a call New Year’s morning alerting him to the emergency.
When Mayschack and Drew Harrell, MD, associate professor in the Department of Emergency Medicine, met up in the parking lot at the base of the Sandia Peak Tramway a short time later, both knew this was a situation they had trained for.
“We had the folks that run the tram reach out to us in the summer of 2020,” Mayschak says. “They basically wanted to set up a plan for how to rescue people from the tram should it get stuck the way that it did.”
 The plan involved a long-standing rescue partnership between the UNM Mountain Medicine team and the Bernalillo County Sheriff’s Office helicopter unit. In this case, the team drew from the experience of Air Zermatt, the helicopter rescue unit serving the region around the Matterhorn in the Swiss Alps.
The plan involved a long-standing rescue partnership between the UNM Mountain Medicine team and the Bernalillo County Sheriff’s Office helicopter unit. In this case, the team drew from the experience of Air Zermatt, the helicopter rescue unit serving the region around the Matterhorn in the Swiss Alps.
“We went out there and did a few iterations using the helicopter to insert people directly into the tram car and how to take people out of the tram car using the helicopter,” Mayschak says.
The procedure entailed attaching two passengers to a rope suspended from beneath a hovering chopper, then flying them down to the base. “We had already worked through the logistics of what that would like and how we would do it,” says Harrell, who is also a reserve deputy with the Sheriff’s Office.
This situation was different. By the time the pair arrived on New Year’s Day, tram operators had managed to inch the car with 20 occupants next to the higher of the two steel towers supporting the cables. Sandia Peak employees and members of the Albuquerque Mountain Rescue Council who had scaled an icy ladder to the top of the tower were preparing to lower the passengers to the ground using harnesses and ropes.
But another problem still needed to be solved: how to bring the passengers down to the tram headquarters from a precarious icy ridge at 8,500 feet in elevation as the weather worsened and dense clouds shrouded the mountainside.
 “We came up with a plan,” Mayschack says. BCSO pilot Larry Koren would land the helicopter on a narrow ledge about 70 yards from the tram tower, load the passengers and fly them down, a few at a time. He flew Mayschak and Harrell up to the tower to coordinate the transfer.
“We came up with a plan,” Mayschack says. BCSO pilot Larry Koren would land the helicopter on a narrow ledge about 70 yards from the tram tower, load the passengers and fly them down, a few at a time. He flew Mayschak and Harrell up to the tower to coordinate the transfer.
They secured the landing zone, but they had to wait for conditions to improve enough for the helicopter to operate. “There was a lot of sitting around waiting for a weather window,” Harrell says. Once Koren felt it was safe to fly, the pair escorted the passengers the helicopter, instructing them how to get onboard and communicated with the pilot when everyone was secure so he could take off.
“We did that – rinse, repeat – eight to nine times, getting all 20 people from the initial tram car down,” Mayschak says, adding that it took another two hours to get the passenger out of the second tram car and back down the mountain.
 “People were very excited to see us,” he says. “Everyone had a big smile on their face because they were no longer in the tram car. By the time we saw them they were through the hardest part of it emotionally. At that point things were starting to look a lot better.”
“People were very excited to see us,” he says. “Everyone had a big smile on their face because they were no longer in the tram car. By the time we saw them they were through the hardest part of it emotionally. At that point things were starting to look a lot better.”
Despite their ordeal, the passengers “were actually in pretty good shape,” Mayschak says. “It was pretty impressive to see that people were not too cold. They had some space blankets, and being huddled up in a car like that kept each other warm to some degree.”
The dramatic rescue drew extensive national attention.
“It’s an interesting situation, in that it seems in some ways kind of monumental to evacuate that many people off the mountain under those conditions,” Mayschak says. “But for us in the moment I think we were all in agreement that because of the training we do regularly and we’re out on the mountain all the time and we’re out in those conditions all the time, it felt like another day of training.”
Harrell agrees. “For us, it was like, ‘Hey, there’s a tram car,’” he says. “We knew that logistically if the weather cleared and if the tram car had not been able to be moved to that tower, that we could get them out.”
Mayschak acknowledges one aspect that stood out as unique, however: “It was definitely a memorable way to start the new year!”
The dramatic New Year's Day rescue of 21 people stranded in a blizzard on the Sandia Peak Tramway -- in which members of the UNM International Mountain Medicine Center played a key role -- attracted international attention.

LoraAnn Lovato
7 years at SRMC
ICU nurse for 12 years
ICU Charge Nurse/Unit Based Educator
The best thing about my job is being able to make a difference in my patient’s lives.
Sometimes there is a happy ending and we can celebrate what the patient has overcome. Other times, there is no happy ending. Nevertheless, I find the beauty in both scenarios.
- LoraAnn Lovato

Harriet Smith, RN
4.5 years at SRMC
10 years total
Inpatient - Medical/Surgical
What do you want people to know about what you do?
The profession is difficult in many ways, and nurses are human. We have emotions and limits, we deserve for grace to be granted to us at times.
- Harriet Smith

Annika Page, RN
3 years at SRMC
8 years nursing total
Inpatient med/surg
Nurses play a vital role in providing health care to New Mexicans, but they are in short supply throughout the state. This map is based on the findings in the 2021 New Mexico Health Care Workforce Report, a summation compiled by the UNM Health Sciences and submitted to the New Mexico Legislature each October 1. As in past years, it shows severe shortages in the number of nurses in nearly every county in the state, offering stark visual evidence of the need for strategies to bolster the nursing workforce.
This page is designed for bigger devices. Please shift to "Desktop site" for better view.